Last summer, Eloise Reynolds paid the bill for her husband’s final stay in the hospital.
In February 2022, doctors said that Kent, her husband of 33 years, was too weak for the routine chemotherapy that had kept his colon cancer at bay since 2018. He was admitted to Barnes-Jewish Hospital in St. Louis, not far from their home in Olivette, Missouri.
Doctors discovered a partial blockage of his bowel, Reynolds said, but she remained hopeful that his treatment would soon resume.
“I remember calling our kids and saying, ‘OK, this is all really good news. We just need to get him kind of bolstered back up and feeling well,'” she said.
MATT KILE FOR KFF HEALTH NEWS
But years of chemotherapy had taken a toll on his body, and he told his wife that he couldn’t go on any longer.
Kent was discharged and began hospice care at home. He died the next month at age 62.
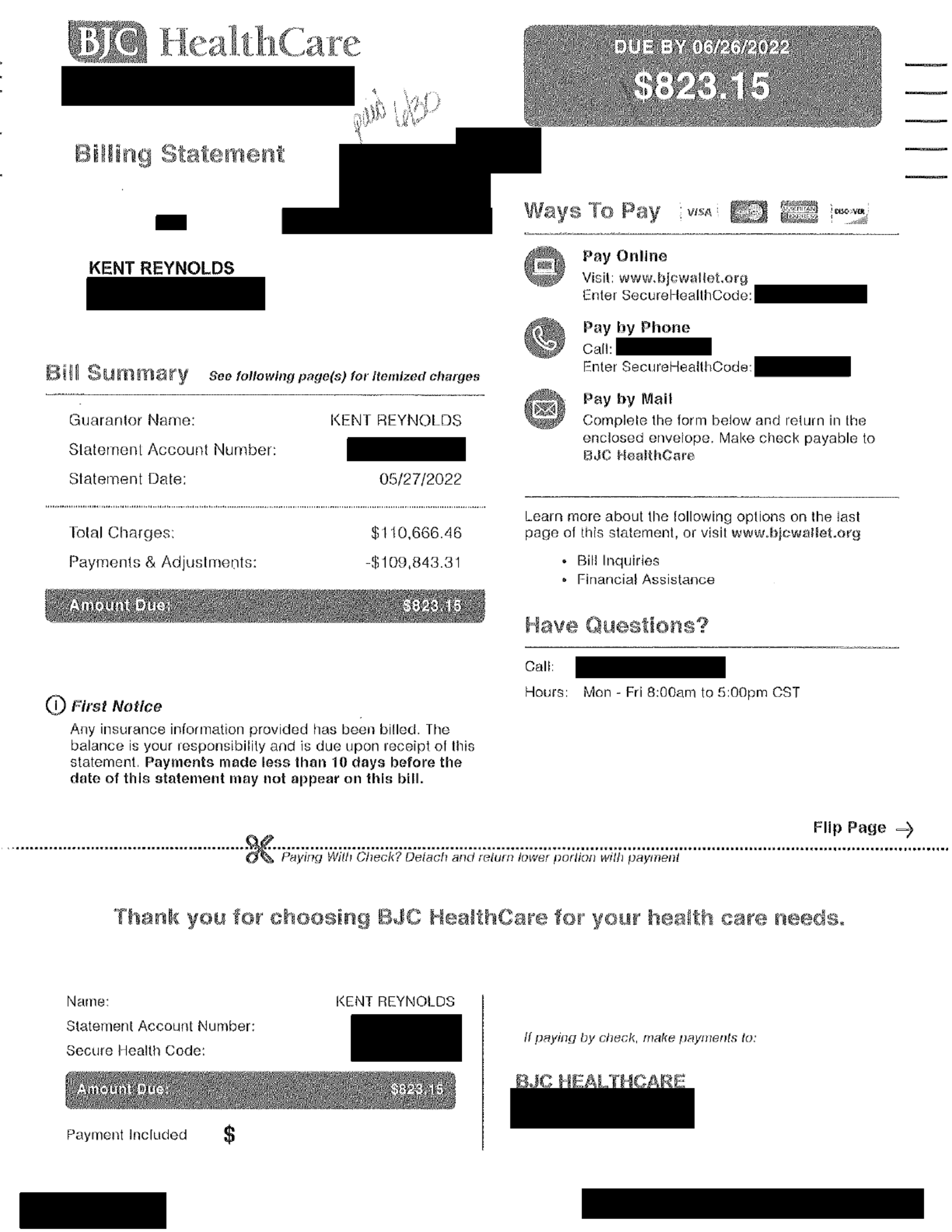
When Reynolds received the bill for the hospital stay, she paid the $823.15 it said her husband owed. She scribbled “paid” on the bill, memorializing the date, June 30, 2022 — the financial endpoint, she thought, of Kent’s years of treatment.
Then the bill came (again).
The Patient: Kent Reynolds, deceased, had been covered by Blue Cross and Blue Shield of Illinois through his Illinois-based employer.
Medical Service: A 14-day hospital stay related to complications from colon cancer, including a partially blocked bowel.
Service Provider: BJC HealthCare, a tax-exempt health system that operates 14 hospitals, mostly in the St. Louis area, including Barnes-Jewish Hospital.
Total Bill: The hospital charged $110,666.46 for the stay before any payments or adjustments. The insurer negotiated that price down to $60,348.77, and Reynolds paid the $823.15 the hospital said the patient owed. Then, a year after her husband’s death, she received a new version of the bill from the hospital, charging her an additional $1,093.16.
What Gives: Reynolds encountered a perplexing reality in medical billing: Providers can — and do — come after patients to collect more money for services months or years after a bill has been paid.
The new bill said Kent Reynolds had been enrolled in a payment plan and that the first “monthly installment” on the nearly $1,100 balance was soon due.
KFF HEALTH NEWS
Patient charged more
She said she called both the hospital and Blue Cross and Blue Shield of Illinois in search of answers but didn’t get an explanation that made sense to her.
According to Reynolds, a BJC HealthCare representative told her that the insurer had paid more than it owed, meaning the health system had to reimburse the insurer and charge the patient more.
Reynolds said she grabbed a yardstick to use as a straight edge and went line by line, comparing both bills, to see what had changed, a task that evoked painful memories of her husband’s last days. The amount for each individual charge — medications, lab tests, supplies, and more — was the same on both bills. The total had not changed.
Only three aspects of the bill had changed: the adjustments; the amount paid by the insurance company; and what the patient owed.
Adjustments, or discounts, are amounts that may be subtracted from a medical bill, typically under the provider’s pre-negotiated contract with an insurer. Insurers and providers agree to lower, in-network rates for services provided to patients covered by the insurer.
Reynolds also received an EOB, or “explanation of benefits,” notice showing the insurer reviewed the bill again in February, a year after the hospital stay. The document said the hospital’s charges for her husband’s private room — amounting to nearly $77,000 — were more than his health plan’s negotiated room rates, which did not cover the full cost.
The EOB noted that the patient could still owe the hospital $50,216.31 for the room charges — a startling amount — although Reynolds ultimately received no bill indicating she owed that much.
Reynolds said she spent hours trying to understand the items on the hospital and insurance paperwork, since they used medical abbreviations and were grouped differently on the documents.
“It shouldn’t be this hard for a widow to figure out what the medical bills were,” said Erin Duffy, a research scientist at the University of Southern California’s Schaeffer Center for Health Policy and Economics.
Blue Cross and Blue Shield of Illinois declined to comment despite receiving a signed release from Reynolds waiving federal privacy protections.
MATT KILE FOR KFF HEALTH NEWS
The Resolution: Unclear about what had changed and how much she owed, Reynolds held off on paying the second bill. After KFF Health News contacted BJC HealthCare, Laura High, a media relations manager for the system, said the charges were the result of a “clerical error.” Reynolds no longer has a balance, High said in an email in May.
“I was shocked by it,” Reynolds said. “I’m convinced most of the people I know would have paid this.”
High did not answer questions about the cause of the billing error or how often such errors occur.
However, Duffy provided a different explanation for the charges. “This doesn’t seem like an error,” she said. “It seems consistent with their insurance plan design.”
She said it appeared the additional $1,100 charge — assessed a year later — represented Kent’s coinsurance share of the private room charges, which she found as a recurring line item on each page of the bill under the heading “Oncology/PVT.”
While his coinsurance responsibility could have amounted to 10% of what the insurer paid in room charges — potentially a huge amount — Kent had met his out-of-pocket payment maximum for the year, so the charges did not reach the full 10% of the room costs, Reynolds said.
The Takeaway: In the United States, medical bills and insurance statements create a burdensome puzzle for patients to sort through to determine what is actually owed. The first rule of thumb is: “Don’t pay the bill before you’ve gotten the EOB,” which is the insurer’s accounting of what you owe and what the insurer will pay, said Kaye Pestaina, co-director of KFF’s Program on Patient and Consumer Protections.
In addition, ask for an itemized breakdown of charges and compare it against the EOB.
Medical billing experts said standardizing terms and other details on medical bills and EOBs would help patients enormously in this undertaking.
A few states have taken steps toward giving patients more information about health care charges, including by simplifying medical bills. In 2019, New York state lawmakers proposed requiring hospitals to provide patients with bills in plain language, including an itemized list of services labeled as paid by the insurer or owed by the patient. The proposal, which did not advance, required hospitals to send patients a single bill within seven days of leaving the hospital.
Medical bills lack oversight
Reynolds’ experience highlights the lack of laws and standards around how long providers have to bill — and review bills — for medical services. Insurers may dictate in their contracts how long providers have to submit claims; the Medicare program has a 12-month limit to file claims, for instance. However, Dave Dillon, a spokesperson for the Missouri Hospital Association, said no laws restrict how long providers have to send a bill to patients.
Creditors may seek payment from a deceased person’s estate to collect whatever they can, said Berneta Haynes, a senior attorney at the National Consumer Law Center. In Missouri, a living spouse can be held responsible for a deceased spouse’s medical bills in certain instances, said Terry Lawson, a managing attorney for Legal Services of Eastern Missouri.
Experts said they did not pinpoint anything Reynolds could have done differently, noting that it is the system that needs to change.
“When can she move on from these hospital bills?” Duffy asked.
KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programs at KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization providing information on health issues to the nation.